Sleep Paralysis
First created | 10/01/1999
Last edited |
- Ohayon MM, Guilleminault C, Priest RG. Night terrors, sleepwalking, and confusional arousals in the general population: their frequency and relationship to other sleep and mental disorders. J Clin Psychiatry 1999;60:268-76; quiz 277.
Sleep Paralysis is a transient and generalized inability to move and speak that occurs during the transitional period between sleep and wakefulness.
Episodes can vary in duration from one to several minutes and are usually extremely distressing for the individual, especially when accompanied by hypnagogic or hypnopompic hallucinations.
HISTORY
Many vivid descriptions of Sleep Paralysis can be found in the literature of the 19th century (in Maupassant's Le Horla and in Melville's Moby Dick, for example) and of the early 20th. The following excerpt is from F. Scott Fitzgerald's The Beautiful and the Damned: "...I lay there, frozen with most awful fears, not daring to drag away my hand; yet ever thinking that I could but stir it one single inch, the horrid spell would be broken" (Fitzgerald, 1922).
Interest in the phenomenon at the time extended beyond the literary sphere, as evidenced by Binns' clinical description of Sleep Paralysis in 1842, one of the earliest on record. The term Sleep Paralysis, however, was introduced only eighty-five years later, in 1928, by Wilson to describe attacks of powerlessness that can occur upon awakening. Two years earlier, in 1926, Adie linked Sleep Paralysis to narcolepsy, an association that persists to this day.
 Before our study, it was estimated that Sleep Paralysis occurred in 30% to 50% of narcoleptic patients (Broughton, 1990; Yoss and Daly, 1967). The prevalence of isolated Sleep Paralysis (i.e., not related to other medical or psychiatric disorders) in the general population was less documented:
Before our study, it was estimated that Sleep Paralysis occurred in 30% to 50% of narcoleptic patients (Broughton, 1990; Yoss and Daly, 1967). The prevalence of isolated Sleep Paralysis (i.e., not related to other medical or psychiatric disorders) in the general population was less documented:
- The earliest studies of the phenomenon involving non-narcoleptic subjects were completed in the early sixties and reported lifetime prevalence rates in narrowly defined populations. For example, Goode (1962) and Everett (1963) observed rates of 4.7% and 15.4%, respectively, for self-reported Sleep Paralysis in a population of medical students.
- Later studies focusing on specific ethnic groups yielded higher rates; such was the case for Bell et al. (1984) who noted a prevalence of 41% among Black Americans.
- In a study of adults living on the northeast coast of Newfoundland, Ness (1978) reported a rate of 62% for attacks of old hag, as Sleep Paralysis is known in that part of Canada; the occurrence of several episodes, however, was rare and apparently affected only about 10% of complainers. In summary, prior to the Sleep-EVAL study, most of the epidemiological data available on Sleep Paralysis were obtained from little samples. Consequently, the true prevalence and associated factors of Sleep Paralysis in the general population remained unknown. Similarly, the association between Sleep Paralysis and other disorders, with the exception of narcolepsy, received little attention:
- Certain case reports have shown that Sleep Paralysis may lead to psychiatric disturbances (Gangdev. 1996, Gangdev and Ramjee, 1996) or may appear following posttraumatic stress disorder.
- Others, still, have suggested an association with panic attacks (Paradis et al., 1997;Bell et al., 1986,1988).
- In addition, it has been found that factors such as stress, fatigue, an irregular life pattern and sleep deprivation may predispose individuals to Sleep Paralysis (Takeuchi et al., 1992).
METHOD
A representative sample of the non-institutionalized general population of Germany and Italy aged 15 years or over (N=8,085) was surveyed by telephone using the Sleep-EVAL questionnaire and the Sleep Questionnaire of Alertness and Wakefulness.
RESULTS
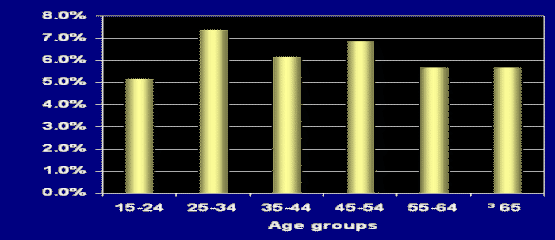
Overall, 6.2% (5.7% to 6.7%) of the sample had experienced at least one Sleep Paralysis episode in their lifetime.
Severe Sleep Paralysis (at least one episode per week) was observed in 0.8% of the sample,
Moderate Sleep Paralysis (at least one episode per month) in 1.4%, and
Mild Sleep Paralysis (less than one episode per month) in 4.0%.
The numerous case reports in the literature of self-injuries, death or murders during episodes of sleepwalking attest to the potentially serious consequences of this sleep problem.
CONCLUSIONS
Significant predictive variables of Sleep Paralysis were:
- anxiolytic medication use,
- memory lapses,
- bipolar disorders, physical disease,
- hypnopompic hallucinations,
- non-restorative sleep and nocturnal leg cramps.
Sleep Paralysis is frequent in the general population, but less than previously reported.
The disorder is often associated with a mental disorder. Users of anxiolytic medication were nearly 5 times as likely to report Sleep Paralysis, even after possible effects of mental and sleep disorders were controlled for. The association between Sleep Paralysis and hypnagogic and hypnopompic hallucinations underlines their common etiology.
REFERENCES
Ohayon MM, Zulley J, Guilleminault C, Smirne S. Prevalence and pathological associations of sleep paralysis in the general population. Neurology 1999;52:1194-200.
