Epidemiological Data on Normal Sleep Patterns
First created | 01/12/1999
Last edited |
Sleep patterns evolve across the normal aging process in complex ways. Changes in sleep patterns across childhood and adolescence, for example, are not only related to chronological age but also to maturational stage. Few studies, however, have made comprehensive analyses of these two aspects in adolescents.
Similarly, chronological age in elderly people does not always match physiological age.
Therefore, changes in sleep patterns may happen earlier, i.e., at a younger age, for some individuals or at an older age for others. Further, epidemiological and other studies suggest that much of the sleep disturbance typically seen in old age is likely the result of medical co-morbidities than age per se (2-6).
Nevertheless, four age-related changes have been consistently demonstrated in polysomnographic (PSG) studies of sleep architecture:
- total sleep time (7-29),
- sleep efficiency (7,9-14,17-23,25-29,30-36), and
- slow wave sleep (7,8,10, 12-18, 21-28, 31,33, 35,37-39) all decrease, while
- wake after sleep onset (12-14,16,17,19,21,23,28,29, 32,33,36,37,40) increases with age.
However, a number of PSG sleep characteristics remain uncertain as regard their evolution with age:
- sleep latency has been reported to increase with age in some studies (10,13,26,31,40), while several other studies found no significant changes with age (8,9,12, 14,16,17,20-23,28,29,32,33,35-37,39,41). Likewise, a number of studies found no significant differences with age for
- percentage of stage 1 (9,25,26,35,39,42) and
- stage 2 (9,13,20,22,23,25,33,35,36,42,43) while many others reported an increase with age of these stages (7,8,12,17,27,28,31).
- Similarly, REM sleep has reported to decrease with age in several studies (7,8,10-12,14,16-18,20,21,23-26,28,31,33,37,38,44) while many other studies found no such association with age (9,13,15,19,22,27,34-36,39-43).
Why such discrepancies between the studies?
Several factors may be responsible for the difficulties identifying age trends in sleep architecture of apparently healthy subjects. For example: small sample sizes; inconsistency in controlling factors that may influence sleep, such as mental or physical illness; uncontrolled use of alcohol, drugs or medications; or insufficient screening for sleep disorders.
WHY STUDYING NORMAL SLEEP PATTERNS?
The knowledge of what can be expected in terms of sleep habits help to make a quick assessment of the "sleep health" of an individual.
For example, anomalies in the sleep duration or in the circadian rhythm
SAMPLES IN THIS STUDY
Representative samples of 10 countries:
EUROPE
- France
- The United Kingdom
- Germany
- Italy
- Portugal
- Spain
- Finland
Target population in Europe: 255.5 M
ASIA
- Korea
Target population: 37.4 M
NORTH AMERICA
- Canada (metropolitan areas of Quebec city, Montreal and Toronto)
Target population: 5.6 M
- United States (states of New York and California)
Target population: 53 M
TOTAL SAMPLE
- 35,475 subjects aged between 18 and 101 years
- 1,429 subjects aged between 15 and 17 years
Total participation rate: 81.3% (Min: 68.1% - Max: 91.4%)
Participants were all interviewed by telephone with Sleep-EVAL
SLEEP CHARACTERISTICS
- Bedtime (night and shift workers excluded)
- Sleep latency
- Nighttime sleep duration
- Wake up time (night and shift workers excluded)
- Daytime sleep
- Extra sleep on week ends
NORMAL DISTRIBUTION OF BEDTIME
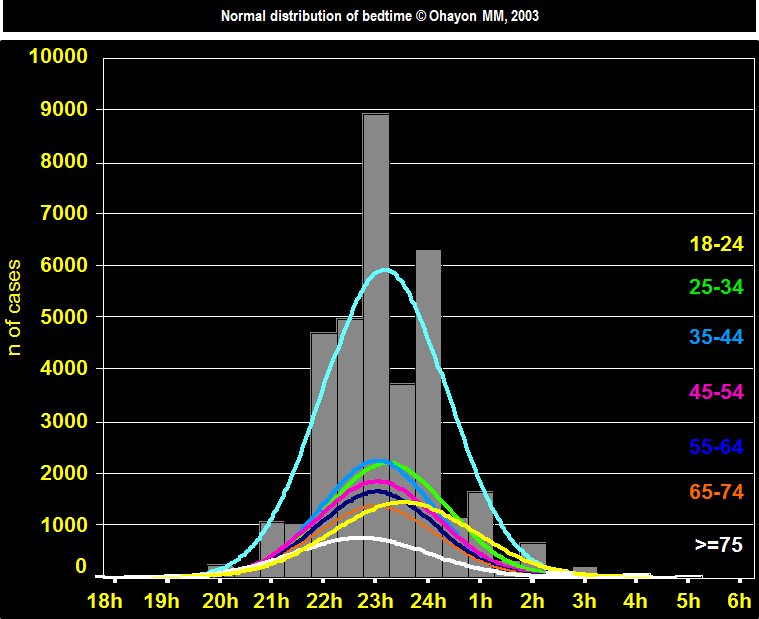
The median bedtime was 23h among all the subjects.
In subjects between 18 and 24 the median was at 23:30 ¨In subjects 75 and older the median was 22:30
BEDTIME (VARIATION BETWEEN COUNTRIES)
The median bedtime in Portugal and Spain was 60 minutes later in all age groups older than 24 years
The median bedtime in France was 30 minutes earlier in age groups older than 44 years.
BEDTIME (EXTREME VALUES)
Early bedtime (5% of the subjects)
- 21:30 or earlier in the subjects between18-54 years
- 21:00 or earlier in the 55 and older
Late bedtime (5% of the subjects):
- 1:30 or later in the 18-34 years
- 1:00 or later in the 35-64 years
- 00:30 or later in the 65 and older
IMPLICATIONS
Bedtime in the extreme values may indicate a circadian rhythm disorder:
- Early bedtime: Advanced sleep-phase syndrome
- Late bedtime: Delayed sleep-phase syndrome
NORMAL DISTRIBUTION OF SLEEP LATENCY
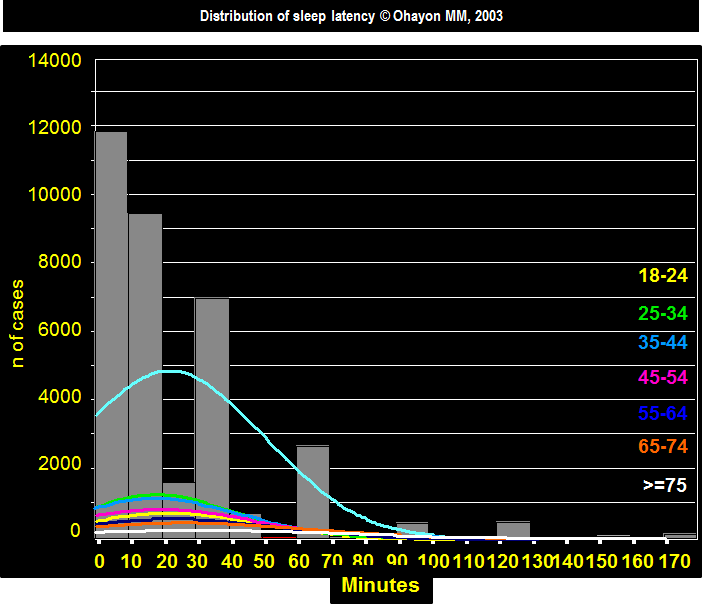
The median sleep latency was 15 minutes for all the subjects
The median was 10 minutes in subjects between 35-54 years and 20 minutes in subjects 75 years and older.
75% of the population is taking 30 minutes or less to fall asleep
SLEEP LATENCY (VARIATION BETWEEN COUNTRIES)
The median bedtime in Portugal and Spain was 60 minutes later in all age groups older than 24 years
The median bedtime in France was 30 minutes earlier in age groups older than 44 years.
SLEEP LATENCY (EXTREME VALUES)
Long sleep latency (5% of the subjects):
- 60 minutes in subjects between 18 and 54 years
- 90 minutes in subjects between 55 and 74
- 120 minutes in subjects 75 years and older
IMPLICATIONS
Defining difficulty initiating sleep as being a sleep latency of more than 30 minutes should be used with caution in general population: 25% of the population is taking more than 30 minutes to fall asleep
NORMAL DISTRIBUTION OF SLEEP DURATION
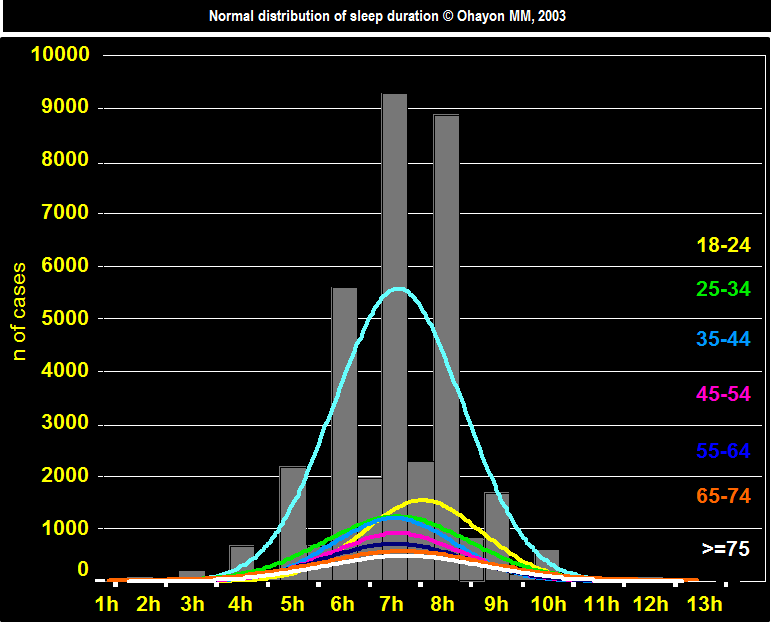
The median nighttime sleep duration was 7 hours for all the subjects.
The median was different of 7 hours only in subjects between 18 and 24 where the median was 7h30 min.
Spanish individuals slept at least 30 minutes more than the other countries.
BEDTIME (VARIATION BETWEEN COUNTRIES)
Short sleep (5% of the subjects):
- 5h or less in subjects between 18 and 64 years
- 4h30 or less in the 65-74
- 4h or less in the 75 and older ¨Long sleep (5% of the subjects)
- 9h or more in the18-34 and 55 and older
- 8h30 or more in the 35-54
NORMAL DISTRIBUTION OF WAKE UP TIME
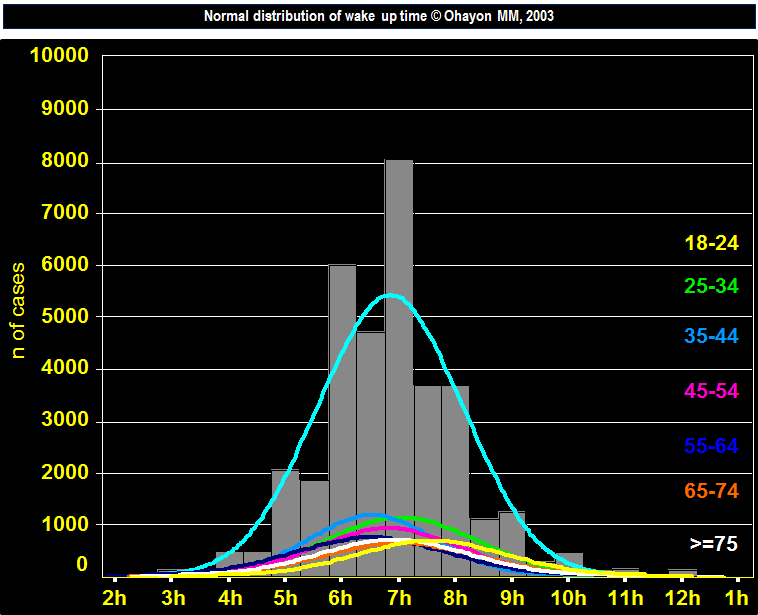
The median wake up time was 7:00 among all subjects.
The median was 7:30 among the 18-24 years.
It was 6:30 among the 35-64 years.
WAKE UP TIME (VARIATION BETWEEN COUNTRIES)
The median wake up time in Portugal and Spain was 30 minutes later in all age groups older than 24 years.
The median wake up time in Germany was 30 minutes earlier in age groups between 18 and 64 years.
WAKE UP TIME (EXTREME VALUES)
Early awakening (5% of the subjects):
- 5:30 or earlier in subjects between 18 and 24 years
- 4:30 or earlier in the 45-64 years
- 5:00 or earlier in subjects 65 and older
Late awakening (5% of the subjects):
- 10:00 or later in the 18-24
- 9:00 or later in the 25-34 and 65 and older
- 8:30 or later in the 35-64
IMPLICATIONS
As for bedtime, wake up time in the extreme values may indicate a circadian rhythm disorder:
- Early wake up time: Advanced sleep-phase syndrome
- Late wake up time : Delayed sleep-phase syndrome
DISTRIBUTION OF DAYTIME SLEEP
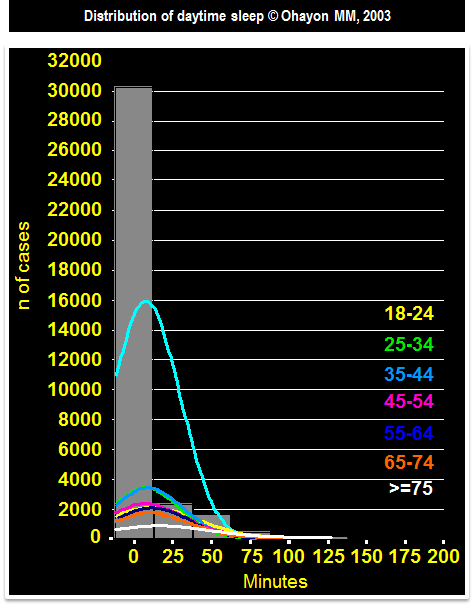
The median duration of daytime sleep was 0 at all age
Long daytime sleep (5% of the subjects): 60 minutes or more in all age groups except in the 35-44 years where the median was 45 minutes
EXTRA SLEEP ON WEEK ENDS
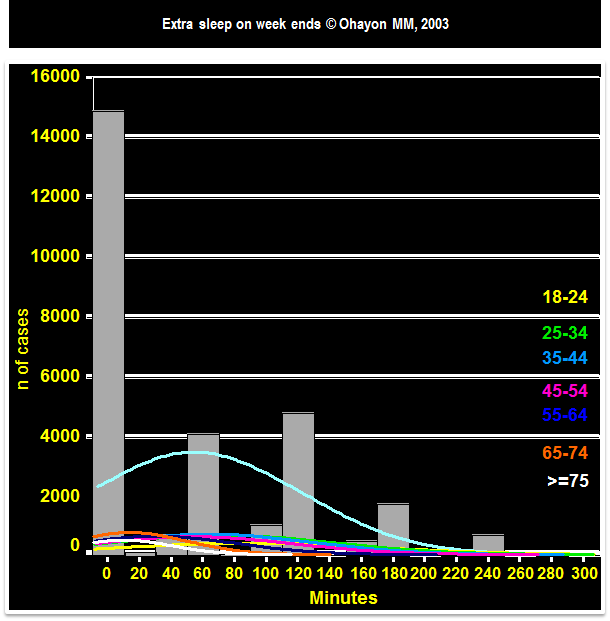
The median extra sleep was 0 minute for all the subjects
The median was:
- 120 minutes in subjects between 18 and 24 years
- 60 minutes in the 25-44 years
- 30 minutes in the 45-54 years
- 0 for subjects 55 years or older
EXTRA SLEEP ON WEEK ENDS (VARIATION BETWEEN COUNTRIES)
Spanish, Portuguese and Italian participants aged between 24 and 54 years had half lower median values of extra sleep than the other countries
EXTRA SLEEP ON WEEK ENDS (EXTREME VALUES)
On week ends and days off, 5% of the participants slept more than:
- 240 minutes in the 18-24 years
- 180 minutes in the 25-54 years
- 120 minutes in the 55-74 years
- 60 minutes in the 75 years and older
Ohayon MM, Carskadon MA, Guilleminault C, Vitiello MV. Meta-analysis of quantitative sleep parameters from childhood to old age in healthy individuals: developing normative sleep values across the human lifespan. Sleep. 2004 Nov 1;27(7):1255-73. Free PMC
